Dr. David Janssen and Dr. William Doubek have spent decades helping women through this journey, guiding each patient through options that fit her body, her goals and her lifestyle. From traditional implant-based reconstruction to advanced pre-pectoral techniques and flap procedures using your own tissue, we offer a full range of reconstructive methods tailored to your unique circumstances.

Breast Reconstruction
Facing a mastectomy is difficult enough without wondering what comes next. At Fox Valley Plastic Surgery, we understand that breast reconstruction is about more than restoring shape. For many women, it’s a meaningful step toward reclaiming their sense of self after cancer treatment.
Breast Reconstruction: Key Details
- Procedure Time: 2-8 hours (varies by technique)
- Anesthesia: General anesthesia
- Recovery: 2-6 weeks initial recovery (varies by technique)
- Results: Final results develop over 3-12 months
- Combination Procedures: Symmetry procedures, nipple reconstruction, fat grafting
What Is Breast Reconstruction?
Breast reconstruction is a surgical procedure that rebuilds the shape and appearance of the breast after mastectomy or lumpectomy. Reconstruction can be performed using breast implants with tissue expansion, your own tissue (called autologous or flap reconstruction), or a combination of both approaches. The right choice depends on many factors, including your body type, cancer treatment plan, personal preferences and lifestyle.
Your team at Fox Valley Plastic Surgery is here to educate and support you throughout your entire journey—explore our Breast Reconstruction YouTube playlist for helpful videos, expert insights, and answers to common questions.
Understanding Your Starting Point
One of the hardest parts of breast reconstruction is understanding where to start. If you’ve recently undergone a lumpectomy or mastectomy, or are facing one of these procedures in the near future, you may not have decided what your next steps are yet. Our surgeons take a thorough approach to evaluating your situation, considering multiple factors like your personal goals, skin and muscle availability, breast asymmetry, and whether radiation or chemotherapy are part of your treatment plan to help determine which approach you might need.
One of the newer aspects of breast reconstruction is figuring out when to do the reconstruction. While immediate reconstruction at the time of mastectomy can be an excellent option for many patients, it is not always the best choice for every individual or every clinical situation. An important factor that significantly influences outcomes is the condition of the skin after mastectomy. Skin that has weeks to recover its blood supply will have fewer complications.
Other factors
Other factors we look at when developing a breast reconstruction plan include:
- Type mastectomy (total or partial)
- Immediate or delayed reconstruction
- Reconstruction type (implants vs. tissue flap)
- If choosing implants, whether a tissue expander is needed first
- Tumor location and what we anticipate the thickness of the skin flap to be after mastectomy (an aspect of reconstruction we have no control over)
At Fox Valley Plastic Surgery, we believe every woman deserves to know her options. Your surgeon will take the time to walk you through each possibility, answer your questions, and help you feel more confident about what comes next. Our goal is to give you clarity and support so you can move forward with a plan that feels right for your body and your life.
Breast Reconstruction at Fox Valley Plastic Surgery
At Fox Valley Plastic Surgery, we offer multiple reconstruction techniques because no single approach works for everyone. Dr. Janssen and Dr. Doubek will evaluate your anatomy, discuss your goals, and recommend the method that gives you the best chance of achieving results you’ll feel confident about.
Reconstruction With Implants
Breast reconstruction with implants is typically done using tissue expanders, which are placed at or within weeks of the mastectomy. Tissue expansion stretches healthy skin to provide coverage for an implant. Reconstruction with tissue expansion allows an easier recovery than flap procedures, but it is a more lengthy reconstruction process. The implant is expanded distantly after placement through an internal valve to expand the skin. A second surgical procedure will be needed to replace the expander, as it is not designed to serve as a permanent implant.
Breast implants can be used in combination with or as an alternative to flap techniques. There are many different types, shapes, sizes, and brands of implants available. During the consultation process, you’ll work with your surgeon and our phenomenal nurses to find the right implant for you. You may also “test out” the implants with our Vectra 3D imaging system, which allows you to visualize your potential results. Depending on your needs and goals, Dr. Janssen or Dr. Doubek may recommend adding fat grafting and nipple and areola reconstruction to your surgical plan. Sometimes the nipple and areola are tattooed instead of reconstructed.
Implant Placement
At Fox Valley Plastic Surgery, we perform pre-pectoral reconstruction, which means that implants are placed over the chest muscle rather than beneath it. This modern approach has become increasingly popular as patients who underwent prepectoral implant reconstruction report higher satisfaction scores in physical and psychological well-being compared to traditional submuscular techniques, according to a 2024 study published by Dr. Janssen, Dr. Doubek and others in the Journal of the American Society of Plastic Surgeons. Additional research has also shown that pre-pectoral reconstruction offers full pectoralis muscle preservation, reduced loss of strength, reduced pain, and elimination of animation deformity.
One & Two-Stage Reconstruction
Breast reconstruction with implants can be accomplished in one or two stages:
- Direct-to-implant reconstruction: The benefit of direct-to-implant reconstruction (also called one-stage reconstruction) is that it usually requires only one surgery. There are specific parameters to be a good candidate for one-stage reconstruction.
- Tissue expander-to-implant reconstruction: This is the most common type of breast implant reconstruction. An expander is placed beneath the skin and muscle. The expander is gradually filled with a saline solution to increase its size. After the skin and muscle over the breast have stretched enough to form a pocket to house the implant, a second procedure removes the expander and places a permanent silicone or saline implant into the newly expanded space.
Autologous Reconstruction Techniques
Although implant-based reconstruction is more common thanks to advances like AlloDerm, flap reconstruction may still be recommended for patients without adequate tissue coverage. Flap techniques use skin, fat and muscle from other areas of the body to rebuild the breast mound, providing natural results and eliminating the potential need for implant replacement or revision.
TRAM Flap
The TRAM (transverse rectus abdominis muscle) flap uses donor fat, muscle and skin from a woman’s abdomen to reconstruct the breast. The flap may remain tethered to the original blood supply and tunneled up through the chest wall, or it may be completely detached and formed into a breast mound using microsurgical techniques. It’s important to understand that taking a muscle flap from the stomach can result in some abdominal wall effects, such as an inability to do sit-ups. These considerations are part of what we discuss during your consultation.
Latissimus Dorsi Flap
The latissimus dorsi flap tunnels muscle, fat and skin attached to its original blood supply from a woman’s back to the chest wall. Occasionally, the flap can reconstruct a complete breast mound, but more commonly, it provides the muscle and tissue necessary to cover and support an implant.
DIEP Flap
The DIEP (deep inferior epigastric perforator) flap is a more advanced technique that uses abdominal skin and fat without sacrificing any muscle. This muscle-sparing approach requires specialized microsurgical training but can result in excellent outcomes with less impact on abdominal strength. DIEPs are not currently performed in this area. This surgery is available in either Madison or Milwaukee with long wait times.
Free Flaps
In some cases where a TRAM flap is not recommended, a free flap using fat, muscle and skin from the buttocks, abdomen or thigh may be used. This requires full detachment from the donor site and blood supply, along with special microsurgical techniques.
What to Expect Throughout the Breast Reconstruction Process

Consultation
Your reconstruction journey begins with a comprehensive consultation where Dr. Janssen or Dr. Doubek will listen carefully to your concerns, evaluate your anatomy and discuss all available options. If you’re still in active cancer treatment, we coordinate closely with your oncology team to ensure the timing is appropriate and your reconstruction plan aligns with your overall care.
During this visit, we’ll also review your medical history, examine your chest and skin quality, and discuss factors like radiation treatment that may influence the best approach for your situation. You’ll leave with a clear understanding of your options and a timeline for moving forward. At the time of consultation, we will also run predictive analytics utilizing what is known as the BRAScore (breast reconstruction risk assessment) tool. This helps us set expectations for complication profiles based on large databases of similar patients with similar health situations.

Preparation
Pre-operative preparation varies depending on your chosen reconstruction method. You may need medical clearance from your primary care physician, lab work, and imaging studies. Patients who smoke or vape must quit at least one month before and after surgery because nicotine use significantly increases the risk of complications and poor wound healing.
We’ll provide detailed instructions about medications to avoid, including aspirin and anti-inflammatory drugs that can increase bleeding. You’ll also need to arrange for someone to drive you home after surgery and help with daily activities during the first few days of recovery.
Procedure
Breast reconstruction may be performed at the ThedaCare Surgery Center, located in the same building as our practice, or in another accredited facility or hospital. You’ll receive general anesthesia to keep you comfortable, with monitoring throughout by a board-certified anesthesiologist. The length of your surgery depends on the reconstruction method. Implant-based procedures typically take one to two hours, while flap procedures may take four to six hours or longer. Depending on your procedure, you may go home the same day or stay overnight for observation.
Some patients may be suitable candidates for having reconstruction at the same time as the mastectomy, which is known as immediate breast reconstruction. In this procedure, after the general surgeon completes the mastectomy, the plastic surgeon begins reconstructing the breast during the same operation. The advantages of immediate breast reconstruction include the possibility of fewer surgeries and waking up with reconstructed breast(s). The patient and surgeon may desire more time to complete the breast cancer treatment before making a decision about undergoing breast reconstruction.
Newer techniques utilizing what is known as sequential immediate reconstruction are done two or three weeks after the mastectomy. This gives the skin time to heal and significantly lowers the risk of complications. In our hands, this technique results in a 50% reduction in complication rates, predicted by the BRAscore.org tool. Truly delayed breast reconstruction can usually be done any time after the mastectomy.
Breast Reconstruction Recovery & Results
Recovery
Recovery varies significantly depending on the type of reconstruction you have. Implant-based procedures generally involve a shorter recovery than flap reconstruction, though both require patience and careful attention to your surgeon’s instructions.
For implant-based reconstruction, surgery and recovery typically occur in two stages. Stage one involves the placement of a tissue expander at some time after the mastectomy. Patients are generally able to return to work in three to four weeks. Stage two involves the removal of tissue expanders and the placement of permanent implants, which is performed as an outpatient surgery. For each stage, pain is usually manageable with prescribed medication, and discomfort improves steadily as healing progresses.
Flap reconstruction involves a longer recovery because you’re healing two surgical sites: the breast and the donor area. Most patients take four to six weeks off work. You’ll have drains at both sites, and activity restrictions are more extensive to protect the delicate blood supply to your new breast tissue. Over time, breast sensation may return.
Results
Your reconstructed breast will look different immediately after surgery, but the final shape develops gradually over several months. Swelling subsides, the tissues soften, and the breast settles into a more natural position. Most patients see their final results within six to 12 months. Breast reconstruction cannot perfectly replace your original breasts, but it can create a natural-looking shape. Most importantly, the reconstructed breast is free of disease and helps restore your body’s contour.
The final results of breast reconstruction following mastectomy can help lessen the physical and emotional impact of mastectomy. Scar lines will improve, although they’ll never disappear completely. There are trade-offs, but most women feel these are small compared to the large improvement in their quality of life and the ability to look and feel whole again.
Long-Term Outlook
Reconstruction results are long-lasting, though your breasts will continue to change naturally over time, just as they would without reconstruction. Weight changes, aging, and gravity all affect reconstructed breasts. Some patients may benefit from revision or touch-up procedures years later to maintain their results.
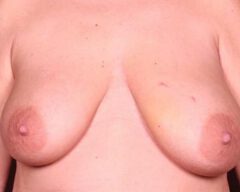
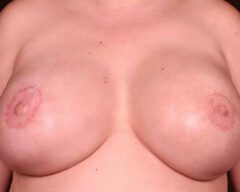
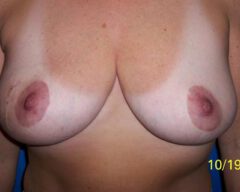
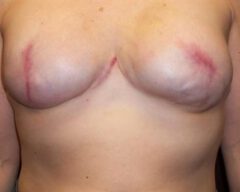
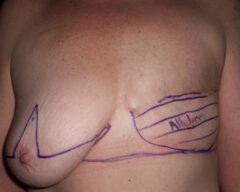
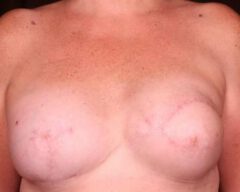
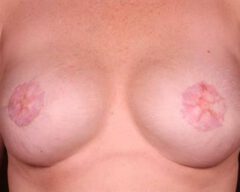
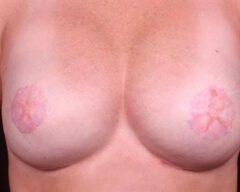
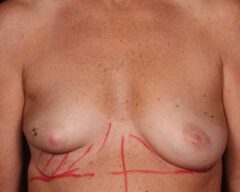
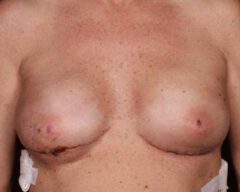
Before & Afters
Discover What’s Possible
Putting the Finishing Touches on Your Reconstruction
Breast reconstruction is often a multi-step process. After the initial procedure to create the breast mound, additional surgeries may be needed to refine breast shape, improve symmetry or restore the nipple and areola.
Nipple Reconstruction
Nipple reconstruction can be performed once your breast mound has healed and settled into its final position, typically three to four months after your initial procedure. The nipple is created using small flaps of tissue from the reconstructed breast itself. This outpatient procedure is usually performed under local anesthesia.
Areola Tattooing
Medical tattooing can recreate the appearance of the areola with realistic color and shading. Tattooing is typically performed after nipple reconstruction and can dramatically enhance the natural appearance of your reconstructed breast. Some patients choose tattooing alone, without nipple reconstruction, and achieve beautiful results.
Symmetry Procedures
If only one breast was reconstructed, you may want a procedure on the opposite breast to achieve better symmetry. This might include a breast lift, breast reduction or breast augmentation, depending on your goals. The Women’s Health and Cancer Rights Act requires insurance coverage for surgery on the opposite breast when performed to create a symmetrical appearance. Unfortunately, many insurance companies are starting to deny this based on the use of artificial intelligence (AI) and considering words like ‘symmetry’ to be cosmetic. This is an evolving situation.
Fat Grafting
Fat transfer can improve breast contour, soften the transition between the implant and chest wall, and fill in areas where the reconstruction may appear uneven. Fat is harvested from another area of your body through liposuction, processed, and carefully injected into the breast. This technique can be particularly helpful for patients with thin skin coverage or visible rippling.
Scar Treatment
After your reconstruction, treatments at the Fox Valley Plastic Surgery Medispa can help minimize scarring and improve overall skin quality. Laser treatments and specialized skincare products can make a noticeable difference in how your scars mature over time.
Aesthetic Flat
There is no absolute need for a woman to have breasts nor total symmetry. Some patients choose to go to what is known as ‘aesthetic flat,’ where they don’t have to worry about the aspects of reconstruction nor the surgeries it involves. Whether or not to preserve nipple/areola will be discussed, which is an operation we are willing to perform for new patients and those who have decided they are done with their implants, especially if they are having discomfort after their reconstruction. Unfortunately, in many of the situations, this is in our radiated patient group. The wound complications are higher after this operation but most feel that it is worth it.
Why Choose Fox Valley Plastic Surgery
For over 30 years, Fox Valley Plastic Surgery has helped women throughout Wisconsin navigate breast reconstruction with compassion, expertise and a commitment to personalized care. Dr. Janssen and Dr. Doubek are board-certified plastic surgeons with decades of experience in reconstructive procedures and know there is no such thing as a cookie-cutter approach when it comes to reconstructing the breasts after lumpectomy or mastectomy.
We also stay at the forefront of reconstructive advances. From the use of the AlloDerm tissue matrix to pre-pectoral techniques that eliminate animation deformity, we continually refine our methods to offer our patients the best possible outcomes. Every recommendation is made with careful attention to your safety, comfort and long-term results, with the goal of helping you move forward with confidence.
Frequently Asked Questions
Is breast reconstruction covered by insurance?
While breast reconstruction is typically covered by health insurance, it is important to understand that this does not mean there are no out-of-pocket costs. Patients are still responsible for applicable copays, deductibles, and any costs not covered by their specific insurance plan.
The Women’s Health and Cancer Rights Act (WHCRA) of 1998 requires most group health insurance plans that cover mastectomy to also cover breast reconstruction. Under WHCRA, your insurance must cover all stages of reconstruction on the breast where you had a mastectomy, surgery on the opposite breast to create symmetry, prostheses, and treatment of complications. Coverage cannot be denied because time has passed since your mastectomy or because you had a different insurance plan when your mastectomy was performed.
What are the risks of breast reconstruction?
All surgery comes with some risk, including breast reconstruction. During your consultation, Dr. Janssen or Dr. Doubek will review these risks in detail to help you make an informed decision. The possible risks of breast reconstruction include, but are not limited to:
- Bleeding
- Infection
- Poor healing of incisions
- Complications related to anesthesia
- Partial or complete loss of flap (for autologous/flap techniques)
- Loss of sensation at donor and reconstruction sites
- Capsular contracture (for implant-based reconstruction)
- Implant rupture
It’s also important for women to understand the risk of breast implant-associated anaplastic large cell lymphoma (BIA-ALCL), a rare type of cancer that can develop in the capsule surrounding a breast implant. BIA-ALCL is not breast cancer but a form of lymphoma. BIA-ALCL is almost exclusively associated with textured implants, with few cases occurring in women with smooth implants. Estimates of the frequency of BIA-ALCL range from 1 in 3,000 to 1 in 50,000+ women. BIA-ALCL grows slowly and can be successfully treated by removing the implants.
Will I need flap reconstruction or tissue expanders?
Flap techniques reposition a woman’s own muscle, fat and skin to create or cover the breast mound. Sometimes, a mastectomy or radiation therapy will leave insufficient tissue on the chest wall to cover and support a breast implant. The use of a breast implant for reconstruction almost always requires either a flap technique or tissue expansion.
Will I have sensation in my reconstructed breast?
Sensation varies from patient to patient. Most women experience some degree of numbness in the reconstructed breast, particularly in the nipple area. Over time, some sensation may return, though it’s usually not the same as before your mastectomy. Flap reconstruction may preserve or restore more sensation than implant-based reconstruction because living tissue is used.
What if I only need reconstruction on one side?
Single-breast reconstruction is very common. To achieve symmetry, you may want a procedure on the opposite breast, such as a lift, reduction or augmentation. Federal law requires insurance to cover surgery on the opposite breast when performed to create a symmetrical appearance after reconstruction.
Will radiation affect my reconstruction?
Radiation can impact reconstruction outcomes, causing tissue tightening, scarring, and changes in skin quality. If you need radiation therapy, your surgeon may recommend delaying reconstruction until radiation is complete, or may suggest specific techniques that perform better after radiation. We coordinate closely with your oncologist to optimize timing and approach.
Schedule Your Consultation Today
If you’re considering breast reconstruction, or if you’ve had reconstruction in the past and want to explore options like pre-pectoral conversion or finishing procedures, we’re here to help. Contact Fox Valley Plastic Surgery at 920-233-1540 to schedule a consultation or complete our online contact form. We serve patients from Green Bay, Fond du Lac, Sheboygan, Appleton and communities throughout Wisconsin.

